WHO has plan how to stop drug-resistant tuberculosis
More than 130,000 lives could be saved if the world implements a strategy to stop drug-resistant tuberculosis.
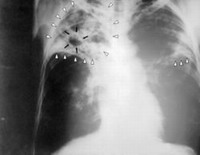
Officials are concerned that the current epidemic - where most people catch curable strains of the disease - might evolve into a drug-resistant variety immune to existing medicines.
"It would be very scary if that happened," said Dr. Ruth McNerney, an infectious diseases expert at London's School of Hygiene and Tropical Medicine. "Tuberculosis would then turn into what it was centuries ago when it was Europe's biggest killer and wiped out generations of people."
The new plan from WHO and the Stop TB Partnership outlines actions they say are needed to slow the spread of multi-drug resistant TB and extensively drug-resistant TB, or XDR-TB.
Drug-resistant TB is primarily a problem in Asia, Africa and eastern Europe, despite the recent trans-Atlantic health scare sparked by Andrew Speaker, an American with XDR-TB who flew to several countries despite being infected.
WHO estimates that US$2.15 billion (1.6 billion EUR) is needed over the next two years to help poor countries tackle issues including disease surveillance, diagnosis and treatment. So far, the health agency says it has about US$640 million (477.7 million EUR).
"We're extremely concerned about multi-drug resistant tuberculosis because we've already got more than 400,000 cases occurring every year," said Dr. Paul Nunn, WHO's tuberculosis, HIV and drug-resistance coordinator. "The evidence we have is that the degree of resistance is increasing over time," he said.
It is also much more expensive to treat resistant TB. Treating regular tuberculosis costs as little as US$16 (12 EUR) for six months per patient. But it costs up to US$15,000 (11,195 EUR) to treat one XDR-TB case for several years - with no guarantee of a cure.
Much depends on how countries on the tuberculosis front lines respond to WHO's new strategy.
"It's early days yet," said Nunn, who says the relative ease of curing regular tuberculosis may complicate efforts to attack the more virulent strains of the disease. "Governments are having difficulty wrapping their heads around why drug-resistant tuberculosis is so much harder to treat."
More than 300 cases of XDR-TB cases have been identified in South Africa, and at least 30 more are picked up each month. Surveys are ongoing in surrounding countries, including Botswana, Lesotho and Swaziland, to determine if the outbreak has jumped borders.
The overstretched health systems in Africa will also be stressed further with the escalating outbreak of drug-resistant TB, being fueled by the AIDS pandemic. "In some hospitals in Africa, you have to empty a bed if you want to treat a new patient," said Dr. Eric Goemaere, head of Medecins Sans Frontieres in South Africa.
WHO's response plan also aims to integrate the treatment of TB and AIDS patients.
"What we're saying is that if you're treating HIV-infected people, then you really must make sure that TB is looked for and rapidly addressed," said Nunn. Because of their weakened immune systems, AIDS patients are more susceptible to TB, which can often prove fatal to them.
Though experts say WHO's strategy is a good start, they are unsure how much of a difference it will ultimately make. "We can try to control the damage that we see today from drug-resistant TB," said Goemaere. "But we are only seeing the tip of the iceberg."
Subscribe to Pravda.Ru Telegram channel, Facebook, RSS!


